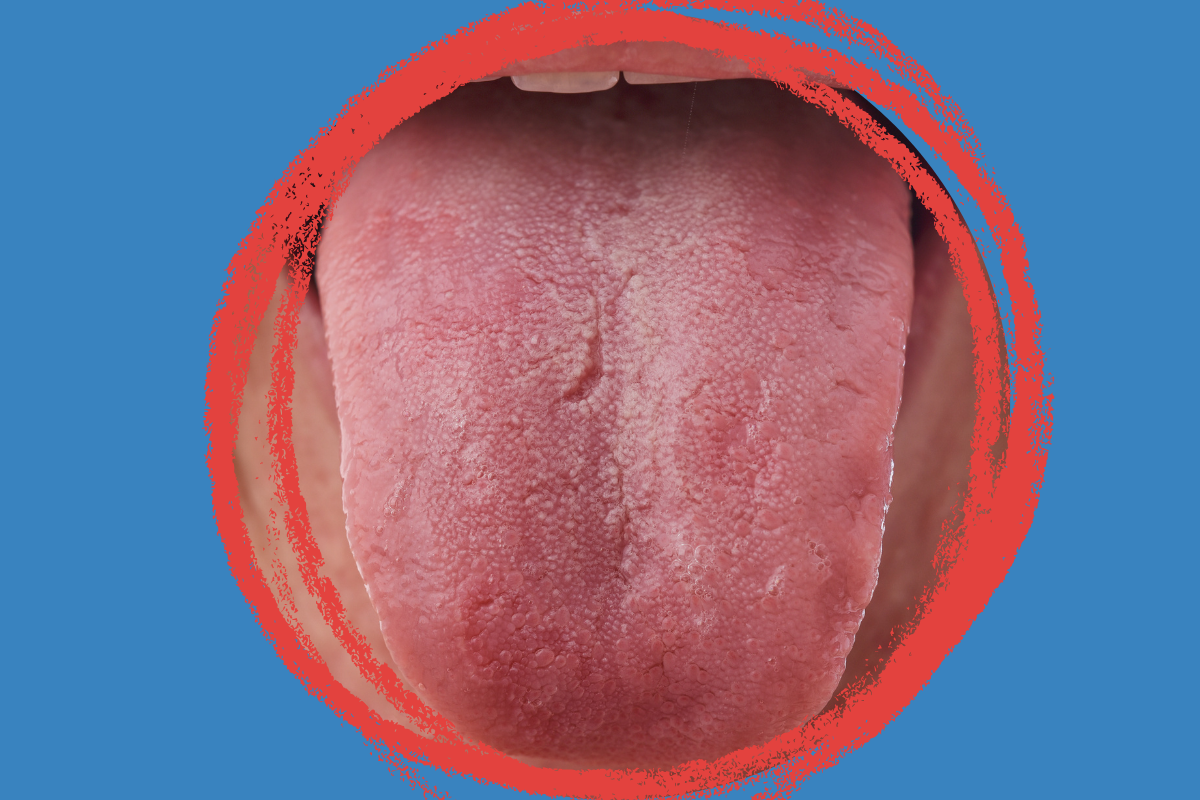
You wake up and your tongue feels like it’s on fire. No ulcer. No redness. No visible injury of any kind — just an unexplained burning sensation in the mouth that won’t go away. You check the mirror. Everything looks completely normal.
If this sounds familiar, you’re not imagining it. What you’re likely experiencing is Burning Mouth Syndrome — a chronic, often frustrating oral condition that affects far more people than most realise, yet remains widely misunderstood and underdiagnosed.
Let’s break down what BMS actually is, why it happens, and what you can do about it.
What Is Burning Mouth Syndrome (BMS)?
BMS syndrome is a chronic pain condition characterised by a persistent burning, scalding, or tingling sensation in the mouth — most commonly affecting the tongue, but also the lips, gums, palate, and throat — without any visible signs of irritation or disease.
The condition is classified into two types:
- Primary BMS: No identifiable underlying medical cause. Believed to involve nerve damage or dysfunction (neuropathic origin).
- Secondary BMS: Directly linked to an underlying condition such as nutritional deficiency, hormonal change, or dry mouth.
BMS is far more common in women — particularly those going through or post-menopause — though it can affect anyone at any age.
Burning Mouth Syndrome Symptoms: More Than Just a Burning Tongue
People with burning mouth syndrome symptoms often describe the sensation as similar to having scalded their mouth with hot coffee — except there’s no burn. Symptoms typically include:
- A continuous burning or hot sensation on the tongue, lips, or gums
- Dry mouth (xerostomia) despite drinking enough water
- Altered taste — metallic, bitter, or loss of taste
- Tingling or numbness in the tongue or mouth
- Soreness that tends to worsen throughout the day and eases with eating or drinking
One key pattern that helps dentists identify BMS: the burning often improves while eating — something that sets it apart from pain caused by ulcers or infections, which typically gets worse with food.
What Causes Burning Mouth Syndrome?
This is where BMS gets complex. There is rarely one single trigger. Burning mouth syndrome causes tend to be multifactorial, and in primary BMS, the exact mechanism is still being studied. That said, identified contributing factors include:
1. Hormonal Changes
One of the most well-established links is between BMS and menopause. Declining oestrogen levels affect the mucous membranes and nerve function in the mouth, making post-menopausal women significantly more susceptible to developing the condition.
2. Nutritional Deficiencies
Low levels of iron, zinc, folate, and vitamins B1, B2, B6, or B12 are frequently associated with oral burning sensation. These nutrients play a direct role in nerve health and saliva production — deficiencies can trigger or worsen BMS significantly.
3. Dry Mouth (Xerostomia)
A persistent dry mouth and burning tongue often go hand in hand. Saliva is the mouth’s natural protective coating. Without adequate saliva, the oral tissues become vulnerable to irritation and nerve hypersensitivity. Dry mouth can itself be caused by medications, autoimmune conditions, or dehydration.
4. Nerve Damage or Dysfunction
In primary BMS, research points to damage or changes in the sensory nerves that supply the mouth — a condition called neuropathic oral pain. The nerves misfire and send pain signals even in the absence of any actual tissue damage. This is similar in nature to other chronic nerve pain conditions.
5. Psychological Factors
Anxiety, depression, and chronic stress have a well-documented relationship with BMS. They don’t cause the condition outright, but they significantly amplify symptom severity and reduce the body’s threshold for pain perception.
6. Other Triggers
- Certain toothpastes or mouth rinses (particularly those with sodium lauryl sulphate)
- Allergic reactions to dental materials
- Acid reflux affecting the oral mucosa
- Poorly fitting dentures causing friction and nerve irritation
How Is BMS Syndrome Diagnosed?
There is no single definitive test for BMS syndrome. Diagnosis is largely one of exclusion — meaning your dentist or specialist will first rule out other oral health conditions before arriving at a BMS diagnosis.
Your dentist will typically review your complete oral health history, examine your mouth thoroughly, and may refer you for blood tests to check vitamin and hormone levels, or to a neurologist if nerve involvement is suspected.
🔍 Conditions that must be ruled out before a BMS diagnosis:
If you’re experiencing unexplained oral pain, a comprehensive dental evaluation is the essential first step. |
Burning Mouth Syndrome Treatment: What Actually Helps?
The honest answer: burning mouth syndrome treatment is rarely a single fix. Because the condition is multifactorial, management is usually tailored to the individual. That said, these are the most evidence-supported approaches:
- Treating the underlying cause: Correcting nutritional deficiencies, adjusting medications that cause dry mouth, treating reflux, or replacing ill-fitting dental appliances often brings significant relief.
- Saliva substitutes and hydration: Staying well-hydrated and using saliva-replacement products can ease dry mouth-related burning considerably.
- Cognitive Behavioural Therapy (CBT): Recognised as one of the most effective interventions for primary BMS, particularly when psychological factors are present.
- Topical treatments: Clonazepam rinses or capsaicin applications have shown benefit in some patients under professional guidance.
- Alpha lipoic acid supplements: Some studies suggest this antioxidant may help with nerve function in BMS patients.
- Lifestyle adjustments: Avoiding spicy foods, alcohol-based mouthwashes, and SLS-containing toothpastes can reduce irritation significantly.
It’s also worth noting that BMS sometimes resolves on its own — but this can take months to years. Waiting it out without a proper diagnosis is not advisable, as secondary causes (like a vitamin deficiency or gum disease) require active treatment.
When Should You See a Dentist for Burning Mouth?
See a dentist if you’ve had a burning tongue without reason for more than two weeks, especially if accompanied by:
- Persistent dry mouth or altered taste
- Visible changes inside the mouth — patches, swelling, or ulcers
- Difficulty eating, swallowing, or speaking
- Worsening symptoms that disrupt daily life or sleep
Don’t try to self-diagnose BMS. Several oral health conditions can produce similar symptoms and require different treatments altogether. Getting a correct diagnosis early makes management far easier and more effective.
The Bottom Line
| Burning Mouth Syndrome is a real, clinically recognised condition — not anxiety, not aging, and certainly not something you should simply live with. If your tongue burns with nothing visible to explain it, that’s your body asking for a closer look.
Whether your BMS is primary or secondary, a dentist with experience in oral medicine can guide you toward the right diagnosis and a management plan that actually works. |
Experiencing persistent mouth burning or unexplained oral pain? Book a consultation at American Dental Practices — our orofacial and oral health specialists in Mumbai and Bangalore are experienced in diagnosing and managing complex conditions like BMS. You don’t have to keep wondering.