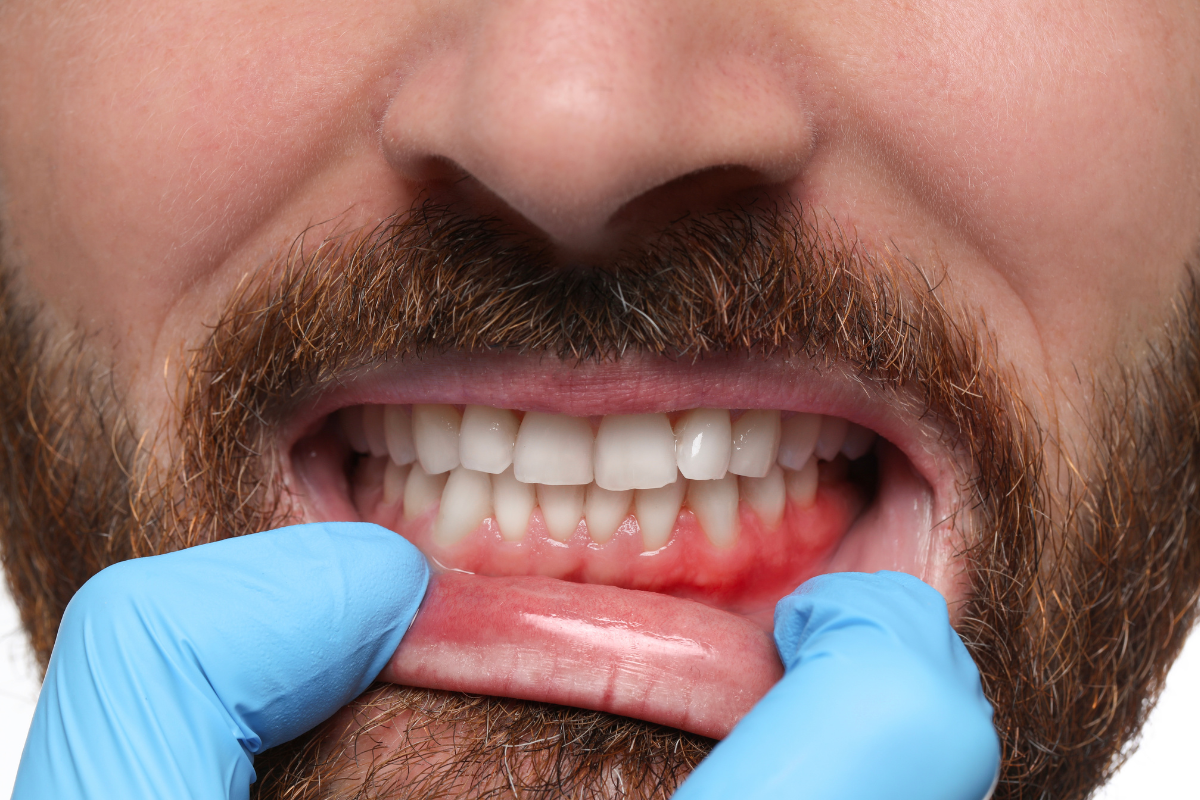
You’re brushing your teeth when something catches your eye — a pale, white patch of gum tissue sitting right around one specific tooth. It wasn’t there last week. Maybe it’s tender, maybe it isn’t, and you’re trying to decide whether to Google it, ignore it, or call your dentist.
The straightforward answer: white gums around a tooth is a symptom, not a single condition. It can mean something as harmless as a canker sore or as urgent as a draining abscess. The appearance, timeline, and accompanying signs are what separate a minor irritation from a genuine dental emergency — and this guide walks you through all of them.
What Do Healthy Gums Actually Look Like?
Healthy gum tissue is firm, coral-pink in colour, and fits snugly around each tooth without gaps or puffiness. It does not bleed during routine brushing, and it sits at a stable level — not visibly creeping down the tooth root. Any deviation from this, particularly white gum tissue around a specific tooth, signals that the area is under some kind of stress and deserves a closer look.
Location is a useful clue: white tissue appearing around a single tooth almost always has a localised cause — infection, trauma, or ulceration. White patches spanning multiple teeth or large areas of the gum may reflect a systemic or chronic condition requiring different investigation altogether.
7 Reasons Your Gums May Be Turning White
1. Canker Sore (Aphthous Ulcer)
The most common and most benign cause. A canker sore on the gum is a shallow oval ulcer with a white or yellowish centre and a defined red border. These appear suddenly — triggered by stress, minor injury from a toothbrush or accidental bite, acidic foods, or hormonal shifts — and are entirely non-contagious.
- Appearance: Small, clearly bordered white/yellow oval with a red rim — looks like a small crater
- Pain: Tender, particularly when touched by food, drink, or the tongue
- Timeline: Self-resolves in 7–14 days without any treatment
- Action needed: None unless it persists beyond two weeks or is unusually large
2. Dental Abscess or Sinus Tract
A dental abscess — bacterial infection at the tooth root — can push through the gum as a small, white dome-shaped bump called a sinus tract or fistula. This forms when the body creates a drainage channel to release pressure from a deep infection. Once it drains, it may feel surprisingly painless — but this is not recovery. The infection is still active and needs professional treatment.
- Appearance: Raised, white or yellowish pimple-like bump near the affected tooth
- Pain: Throbbing when blocked; may ease temporarily once the tract opens
- Other signs: Persistent bad taste, sensitivity to pressure or temperature, swollen jaw in severe cases
- Action needed: Urgent — requires root canal treatment or extraction. Will not heal without professional care
3. Gum Disease (Periodontitis)
Advanced gum disease causes the gum tissue to recede, thin, and pale — sometimes appearing white or translucent at the margins where it pulls away from the tooth. In its most severe acute form, gum tissue can develop greyish-white necrotic patches accompanied by significant pain, bleeding, and a distinctive foul odour.
- Appearance: Pale, receding gum margin; white plaque deposits at tooth base; possible necrotic patches in acute cases
- Other signs: Bleeding when brushing, chronic bad breath — signs covered in detail in our natural mouthwash and bad breath guide
- Action needed: Professional scaling, root planing, and laser gum treatment in advanced cases — home care cannot reverse established periodontitis
4. Leukoplakia
Leukoplakia is a thick white patch that adheres firmly to the gum or oral lining and cannot be wiped off — the key characteristic that separates it from oral thrush. Most commonly linked to tobacco use in any form, it can occasionally develop without an obvious trigger. While many cases are benign, a percentage carry pre-cancerous or cancerous change — making this the one cause on this list where immediate evaluation is non-negotiable.
- Appearance: Flat or slightly raised, firm white patch — rough or wrinkled texture, does not rub away
- Pain: Usually completely painless — which is why it frequently goes unnoticed
- Action needed: Dental evaluation and biopsy if present for more than two weeks. Do not delay
5. Oral Thrush (Candida Overgrowth)
Oral thrush produces creamy-white patches on gum tissue caused by Candida fungal overgrowth. Unlike leukoplakia, these patches can be wiped off — leaving a red, raw surface underneath. Most common in patients on antibiotics, inhaled corticosteroids, those who are immunocompromised, or those with poorly controlled diabetes.
- Action needed: Antifungal medication from a dentist or physician, alongside addressing the underlying risk factor
6. Trauma or Chemical Irritation
Aggressive brushing, a sharp food fragment, or chemical irritation from whitening toothpastes and high-alcohol mouthwashes can cause localised white gum tissue as surface cells slough off. This is a strong reason to use gentle, alcohol-free oral care products — particularly around sensitive gum margins.
- Timeline: Resolves within 3–7 days once the offending cause is removed
- Action needed: Remove the irritant, switch to a soft toothbrush, and monitor for healing
7. Normal Post-Extraction Healing Tissue
If you’ve recently had a tooth removed, a whitish layer in and around the socket is entirely normal — it is fibrin healing tissue, not infection. We cover this in detail in our tooth extraction and dry socket guide. The exception: if white appearance is accompanied by worsening pain, swelling, or fever after day three, that warrants an immediate review.
Quick Guide: Can You Wipe It Off?
The single fastest way to narrow down the cause at home — gently try to wipe the white area with a damp gauze or cloth:
| Cause | Wipe Off? | Painful? | Action |
|---|---|---|---|
| Canker Sore | No | Yes | Monitor 2 weeks |
| Abscess / Fistula | No | Yes / No | See dentist urgently |
| Gum Disease | No | Variable | Professional treatment |
| Leukoplakia | No | No | Immediate evaluation |
| Oral Thrush | Yes | Mild | Antifungal medication |
| Trauma / Burn | No | Mild | Remove irritant; monitor |
| Post-Extraction | No | Mild | Review if worsening day 3+ |
White Gums After Brushing — Is That Different?
Many patients notice white gums immediately after brushing that fade within a few minutes. In most cases, this is a temporary surface response — friction or toothpaste chemistry causing brief whitening of the outer gum layer. Generally harmless if it resolves quickly.
However, if you also notice gum recession — the gum line visibly lowering, exposing more of the tooth root — this is a structural change that does not reverse on its own. Recession requires professional gum treatment to halt progression, and can be connected to the tooth sensitivity many patients experience when root surfaces become exposed.
When to See a Dentist — Do Not Wait
🚨 Book an appointment promptly if:
These are not situations where waiting and hoping helps. Early intervention is consistently simpler, faster, and less expensive than treating a problem that has been allowed to progress. |
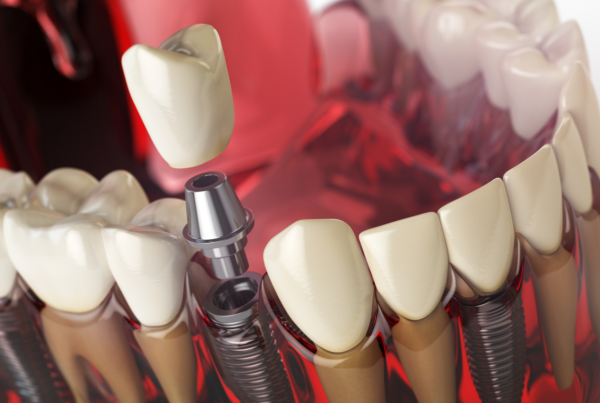
Where the underlying tooth cannot be saved, dental implants remain the most natural-feeling and bone-preserving replacement — and our crown vs veneer guide is worth reading if restoration aesthetics are part of your consideration.
Keeping Your Gums Healthy: Prevention First
Most causes of white gums are significantly reduced by consistent oral care and regular professional check-ups:
- Brush twice daily with a soft-bristled brush — aggressive pressure is a leading cause of gum trauma and recession
- Floss once daily — the only reliable way to remove bacteria from between teeth where gum disease begins
- Choose alcohol-free mouthwash — high-alcohol rinses erode the mucosal lining and worsen sensitivity over time
- Quit tobacco in all forms — the single most impactful change for gum health and oral cancer prevention
- Attend check-ups every 6 months — conditions like leukoplakia and early periodontitis are detectable before symptoms appear
For a complete daily routine that supports long-term gum and tooth health, our oral hygiene guide covers everything from brushing technique to diet.
The Bottom Line
| White gums around one tooth are worth taking seriously — not with panic, but with clear-eyed attention. Most causes are treatable. Many are preventable. A small number require urgent care. The universal rule: any white patch that hasn’t resolved in 14 days needs professional evaluation, without exception.
Your gums are one of the earliest indicators of your overall oral health. Don’t ignore them. |
Noticed white gum tissue around a tooth and not sure what’s causing it? Book a consultation at American Dental Practices in Mumbai or Bangalore. Our team will examine the area, give you a clear diagnosis, and provide same-day gum treatment or specialist referral where needed.